Billing inaccuracies can be disastrous for your large practice’s financial growth. For 10+ years in billing and denial management, Accuramed Billing is known for mitigating the lost revenue and reducing claim denials by 97% for large practices. Available in all 50 States!

Faster and More Cash Inflow

Billing and Coding Accuracy

Improve Patient Experience

End-to-End Denial Management

Compliance Regulation

Cost Savings
These key metrics form the foundation of the revenue cycle management (RCM) workflow, guiding the billing process and overall financial operations of large medical practices. Together, they provide clear insight into performance, efficiency, and revenue optimization across the entire revenue cycle.
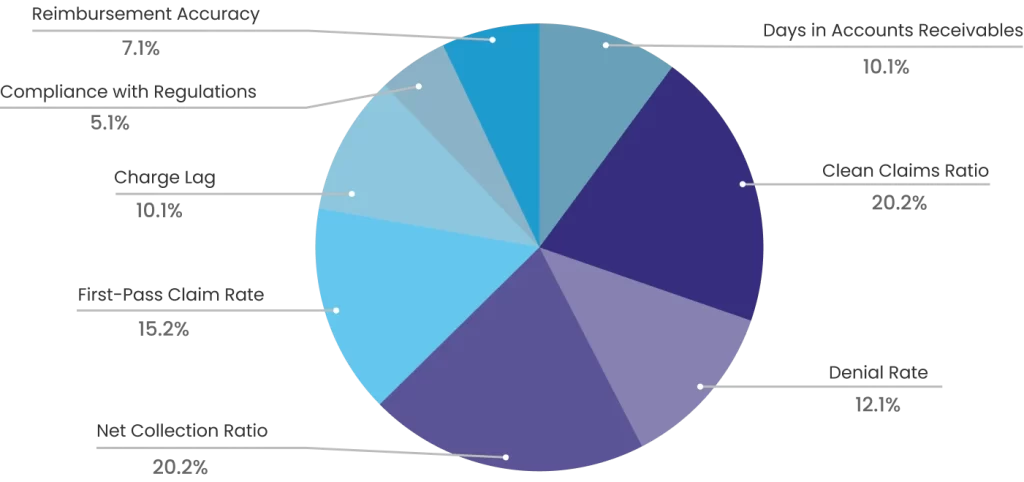
These metrics account for 60% of your billing process’s overall efficiency, productivity, and financial performance. The data is derived from the direct experiences of our clients, reflecting real-world results and actionable insights for optimizing revenue cycle management.
Accounts receivable refers to tracking claims while monitoring the average number of days a practice takes to collect payments. At Accuramed, we maintain a low accounts receivable days ratio, ensuring faster reimbursements and improved cash flow for your practice.
Also referred to as the first-pass clean claim rate, this metric measures how many claims are accepted upon their initial submission. Accuramed delivers high-quality revenue cycle management services designed to maximize your first-pass clean claim rate, reducing rework and accelerating reimbursements.
The net collection rate reflects the total payments collected from both patients and insurers. At Accuramed, we ensure timely payment collection and strive to maintain a high net collection rate, optimizing your practice’s revenue performance.
The claim denial ratio indicates how efficiently your revenue cycle management process is performing. At Accuramed, we actively follow up on denied claims, identify and correct errors, and implement solutions to maximize revenue generation for your practice.
At Accuramed, we recognize that one-size solutions don’t work for large medical practices. That’s why we provide customized, transparent services designed to be error-free. We audit your billing processes, identify and correct mistakes, and review all unpaid or aging claims to optimize your revenue cycle.
Managing a large practice involves multiple challenges—from patient registration to claims submission and denial management. We take over these non-clinical tasks, allowing you to focus entirely on delivering exceptional patient care.
Our integrated billing, coding, and RCM systems are built for large practices. We consistently submit clean claims over 99% of the time, ensure timely claim submissions, follow up on aging accounts receivable daily, and work diligently to maximize reimbursements.
